Rheumatoid arthritis and the foot
Rheumatoid arthritis is an autoimmune disease that is characterised by inflammation, particularly inflammation of the small joints affecting the hands, wrists, feet, and ankles. There is no cure for rheumatoid arthritis; however, the symptoms of the disease can be effectively managed with medication and intervention from podiatry and other health professionals. The earlier rheumatoid arthritis is diagnosed the better it is managed.
What is rheumatoid arthritis?
Rheumatoid arthritis is a chronic, systemic, autoimmune disease that affects the joints and connective tissues. Chronic means that there is no cure for the condition, and systemic means that it has effects on the whole body. Rheumatoid arthritis is characterised by inflammation, which results in swollen, stiff, and painful joints, particularly the joints of the hands, wrists, feet, and ankles. As well as joint stiffness, rheumatoid arthritis can make you feel very tired, making activities of daily living difficult.
What causes rheumatoid arthritis?
Rheumatoid arthritis is an autoimmune disease; this means that the body attacks itself. In the case of rheumatoid arthritis the immune system, which usually destroys bacteria and viruses, destroys the tissue that lines the joints, resulting in pain, inflammation, and stiffness. The exact reason as to why the body attacks itself is unknown, however, it is thought that a combination of both genetic and environmental factors contribute to its development. What is known is that certain factors can increase the risk of developing rheumatoid arthritis, and these include:
- Smoking
- Drinking lots of coffee
- Female aged 30 or over
- Eating lots of red meat
If any of the above risk factors apply to you it does not mean that you will develop rheumatoid arthritis, it just means that your risk may be increased.

How can rheumatoid arthritis affect the feet?
Foot problems are common among those with rheumatoid arthritis, in fact, 90% of people diagnosed with rheumatoid arthritis will develop a foot problem that is associated with their condition. Foot problems associated with rheumatoid arthritis include:
- Joint stiffness
- Inflammation
- Difficulty walking
- Diminished fat pad beneath the feet
- Prominent metatarsal heads (ball of foot)
- Change in foot shape
- Corns
- Callus
- Bursitis
- Ulceration
- Difficulty finding footwear
Foot problems associated with rheumatoid arthritis occur for a number of reasons, for example, some are manifestations of the disease itself, such as joint pain and changes in foot shape, whereas others are associated with medications used in disease management.
The effect rheumatoid arthritis can have on foot shape is the result of inflammation of the joints within the foot. When a joint becomes inflamed the ligaments and joint capsule that surrounds the joint and that hold the joint in place are stretched, the disease process also causes the supporting structures to degenerate. When the joint capsule and ligaments are stretched the bones that form the joint are not securely in place, and this means that they move out of position. The result is that the foot changes shape, due to the bones moving position, and degeneration of the supporting structures of the feet.
What are the signs and symptoms of rheumatoid arthritis?
If you have rheumatoid arthritis you may experience the following signs and symptoms:
- Painful , swollen and stiff joints, particularly the small joints of the hands and feet
- Joint pain is often symmetrical, affecting the same joint on the opposite side of the body
- Anaemia
- Depression
- Fatigue
- Night sweats
- General feeling of being unwell, flu like symptoms.
- Wight loss
- Nodules eyes may become inflamed
- Inflammation elsewhere in the body (e.g. lungs), however, this is less common
Rheumatoid arthritis is a disease that is typically slow to progress; however, there are some people in which the disease progresses much quicker. If you are experiencing any of the above signs and symptoms you should visit your GP, this is because research shows that the sooner the disease is diagnosed and managed, the better the treatment effects will be.
How is rheumatoid arthritis diagnosed?
If you think you may have rheumatoid arthritis you should visit your GP. Your GP will examine your joints and ask you about your symptoms. If the GP thinks that you have rheumatoid arthritis you will be referred to a rheumatologist. A rheumatologist is a doctor that specialises in rheumatic conditions, such as rheumatoid arthritis. Diagnosis is made using blood tests, a physical examination of the joints, your symptoms, and X-ray.
Benefits of podiatry for a person with rheumatoid arthritis
If you have rheumatoid arthritis and it is affecting your feet podiatry will benefit you. The following benefits can be achieved with podiatric intervention:
- Reduction in foot related pain
- Maintain or improve foot function
- Maintain or improve mobility
- Improved skin condition
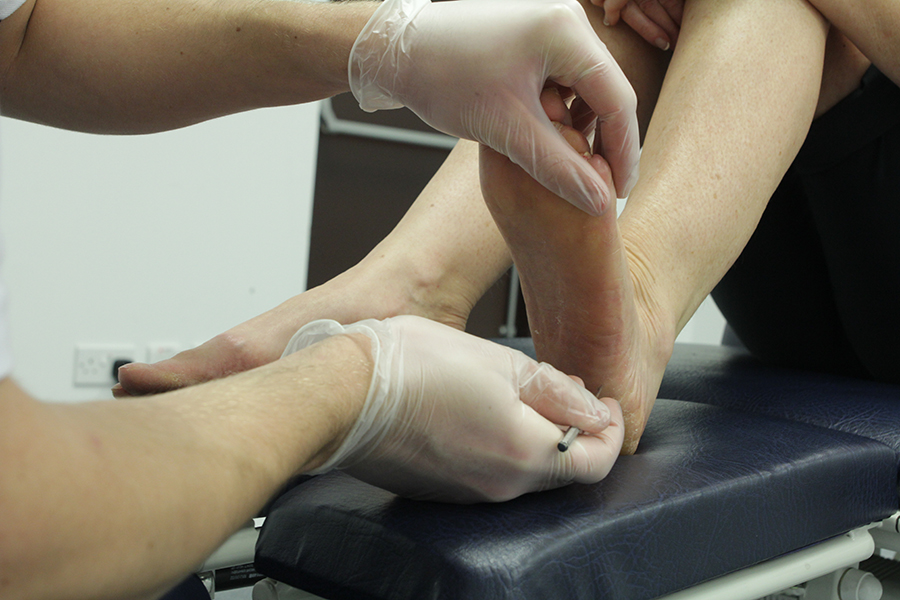
What would podiatry for my rheumatoid arthritis involve?
If you have rheumatoid arthritis and it is affecting your feet please visit a podiatrist. At Chiropody.co.uk an initial consultation would begin with an assessment. During the assessment topics such as medical history, medication, and your foot symptoms will be discussed. The podiatrist will ask you what you would like to achieve, they will then examine the foot and formulate a treatment plan. Treatment will be mutually agreed, and the podiatrist will inform you of what can be achieved. Treatment may include:
Summary
Rheumatoid arthritis is a chronic, systemic, autoimmune disease that is characterised by inflammation. Rheumatoid arthritis affects the joints, particularly the small joints of the hands, wrists, feet, and ankles. The majority of people with rheumatoid arthritis will develop problems with their feet as a consequence of their condition. Podiatry can help you if you are experiencing problems with your feet, by providing treatment and advice that is designed to improve any pain, and increase or maintain your mobility.
To arrange an assessment with one our podiatrists please email office@chiropody.co.uk or call 0330 088 4222.
Save 5% by booking an appointment online.



We work with:

Individuals

Organisations

Health professionals
Get in Touch!
0330 088 4222
If you would like to speak to one of our specialists then please complete this form.
We are open 7 days a week